Human immunodeficiency virus (HIV) has long been regarded as a silent invader, but recent studies have shed light on the virus’s ability to persist within our immune cells, even during active treatment. Virologists have discovered that tiny fragments of HIV’s genetic material, known as viral RNA, can remain inside immune cells despite efforts to suppress the virus’s replication. Although these remnants are not infectious, they may still have consequences for the immune system, potentially causing irritation and exhaustion. This revelation challenges our understanding of the dormant nature of HIV and emphasizes the need for further research in this field.
Contrary to the assumption that antiretroviral drugs completely eliminate HIV from the body, these medications only temporarily halt the virus’s reproduction within immune cells. By acting as a ‘snooze button,’ these drugs prevent HIV from replicating in the ‘helper T’ type immune cells as long as the therapy is sustained. While this approach leads to a significant decrease in the number of detectable HIV particles in the bloodstream, it does not eliminate all traces of viral RNA hidden within immune cells, as indicated by two recent studies. These persistent remnants of HIV’s genetic material may cause a range of effects on the immune system, potentially leading to inflammation and other complications.
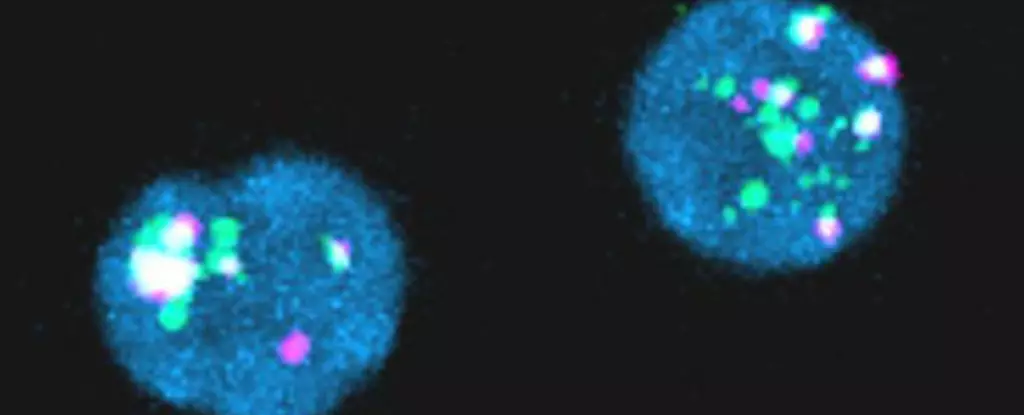
In one study, researchers examined the blood samples of 18 individuals undergoing HIV treatment. They focused on identifying fragments of HIV genetic material within millions of helper T cells using fluorescent RNA probes. Surprisingly, 14 out of the 18 participants had reservoirs of viral RNA, and seven individuals even exhibited production of viral proteins, including an essential component of HIV’s structure called p24. These findings suggested that small amounts of so-called ‘junk’ HIV genetic material can provoke an immune response. Furthermore, the study revealed that the larger the reservoir of HIV gene debris, the more intense the body’s response, indicating a potential link between HIV persistence and immune activity.
Another study reaffirmed these findings by confirming the presence of viral RNA in the helper T cells of individuals undergoing HIV treatment. Moreover, it demonstrated that these remnants hindered the development of CD8+ T type immune cells, which play a crucial role in fighting HIV infection. The researchers highlighted the significance of these findings in terms of the detrimental effect of immune activation, shedding light on the possible long-term consequences of living with HIV.
The implications of these studies extend beyond scientific curiosity, as they carry potential ramifications for the well-being of individuals living with HIV. The presence of persistent viral RNA and its interaction with the immune system may contribute to the negative consequences experienced by some HIV patients, even in cases where antiretroviral therapy is successful. Conditions such as accelerated cardiac disease, frailty, and premature osteoporosis have been associated with long-term HIV infection, suggesting that immune activation caused by the remnants of HIV’s genetic material could be a contributing factor.
Despite these recent developments, many questions regarding the persistence of HIV in the human body remain unanswered. Researchers are eager to understand whether the immune response triggered by the viral remnants is beneficial or detrimental to the individual. Moreover, the potential role of inflammation caused by the persisting viral RNA requires thorough investigation, as its presence may have long-term consequences for those living with HIV.
The discovery of HIV’s ability to persist within immune cells challenges our previous understanding of the virus’s dormancy. The fragments of viral RNA that remain despite treatment signify an ongoing interaction between HIV and the immune system. The consequences of this interaction are still not fully understood and require further research to illuminate the underlying mechanisms. Consequently, these findings open new avenues for the development of more effective treatments and interventions to improve the long-term outcomes of individuals living with HIV.

Leave a Reply